What it is: Sciatica is nerve pain radiating from the lower back down the leg, often caused by nerve root compression or inflammation. The Symptoms: Sharp “electric” pain, numbness, or weakness that fluctuates with position. The Square One Approach: We move beyond temporary “adjustments.” Our protocol focuses on neural desensitisation and active loading to build long-term spinal resilience. Recovery Goal: To transition from pain management to high-performance living without dependency on frequent clinic visits. Looking for a sciatica chiropractor in Singapore? You’re probably dealing with sharp, electric-like pain shooting down your leg, numbness in your foot, or that dreaded feeling that your leg might give out when you walk. Maybe you’ve tried chiropractic adjustments, massage, heat packs, or stretching, and nothing seems to work.Why? Here’s what most people don’t realise: sciatica isn’t just another type of back pain. It’s nerve pain. Nerve pain behaves differently from muscle or even joint pain, and requires a completely different treatment approach. At Square One Active Recovery, we specialise in nerve-specific rehabilitation that addresses why your sciatica keeps coming back. Not just when it hurts. Sciatica is a condition characterised by pain radiating along the sciatic nerve, typically (but not always) caused by nerve root compression in the lumbar spine. This is why some doctors refer to it as Lumbar Radiculopathy, understanding the distinction changes how we approach your rehab. If you’ve landed on this page searching for a chiropractor for sciatica in Singapore, chances are you’ve already noticed that your symptoms behave strangely. The pain travels. It changes with position. Some days it’s your calf, other days it’s your glute. It is hard to pinpoint what exactly you are feeling. That’s because sciatica is a neural symptom, not just a mechanical one. The sciatic nerve is the largest nerve in your body. It runs from your lower back all the way down to your foot! When it becomes irritated, compressed, or inflamed, it sends signals that can manifest as pain, numbness, or tingling, anywhere along its pathway. While every case we see at our Singapore clinic is unique, most patients with sciatica or lumbar radiculopathy experience one or more of the following symptoms: Unlike mechanical back pain, which tends to be dull and localised to the low back, sciatica often feels neurological. Because it is! And that’s why the traditional chiropractic “adjustment” approach often provides only fleeting relief. Many patients come to our Singapore clinic unsure if their leg pain is related to a back strain or true sciatica. Because sciatica involves the body’s largest nerve, the symptoms are often more volatile and neurological than standard mechanical back pain. To help you identify what you might be experiencing, we’ve broken down the key differences below: Traditional spinal adjustments often fail to provide long-term sciatica relief because they focus on joint cavitation (cracking) rather than the underlying neurological and functional causes of nerve irritation. While an adjustment may offer temporary pain relief through a short-term analgesic effect, it does not resolve the mechanical or chemical factors affecting the sciatic nerve. The 4 Real Drivers of Sciatica Pain: A spinal manipulation might create a short-term analgesic effect and temporarily dulls the pain. However, it doesn’t address neural sensitivity, muscular weakness, or faulty movement mechanics to keep you pain-free. This is why our recovery plans focus on progressive loading and strengthening your body to handle the demands of your daily life. When people search for a sciatica chiropractor in Singapore, many have been told they have a herniated disc or “slipped disc“. Let’s clarify what this actually means and why understanding it changes how we treat you. Here’s what modern research tells us: What this means for treatment: If the pain is primarily chemical inflammation, no amount of spinal “realignment” will help. What does help: At Square One, we don’t chase the disc on your MRI scan. We address the mechanical and chemical environment that’s keeping your nerve irritated and painful. We give your body the conditions it needs to heal naturally. At Square One Active Recovery, we treat sciatica as a nervous system issue rather than just a spinal alignment problem. Our evidence-based protocol moves beyond temporary relief by focusing on two essential pillars of recovery: desensitising the nerve and building physical capacity. When sciatic pain is chronic, the nerve becomes hypersensitive. Our first priority is to “lower the volume” of these pain signals through: This phase is about control. You learn how to modulate your symptoms without relying on someone else to “fix” you. Most sciatica treatments in Singapore stop once the pain is gone. At Square One, we believe that absence of pain is not the same as presence of health. To prevent recurrence, we build your “muscular armor” through: Posterior Chain Strengthening: Utilising deadlifts, squats, and carries to fortify the muscles that protect your spine. We meet you where you are. Your journey might begin with gentle mat-based movements or Clinical Pilates on the reformer to build stability while lying down. As you progress, we transition to the Pilates Cadillac for advanced spinal control, eventually graduating to Strength and Conditioning with free weights to make your body “antifragile.” By the time you complete this phase, your spine and surrounding muscles are strong enough to handle real life. This is the “missing piece” in traditional chiropractic. Our methodology doesn’t stop until your results are permanent. Most traditional sciatica treatments in Singapore focus solely on symptom relief. At Square One, we recognise that once your nerve settles down, the real work begins. By training your spine and surrounding muscles to handle the demands of real life, we bridge the gap between “feeling better” and “staying better.” Located at the intersection of Singapore’s CBD and Chinatown, our clinic is designed for busy professionals. Whether you are coming from Raffles Place or 18 Cross Street, our evidence-based process ensures your sciatica treatment is efficient, results-oriented, and sustainable. We begin by identifying your specific functional limitations. Are you struggling to sit through meetings at the office, or is your goal to return to heavy lifting at the gym? We move beyond the diagnosis to understand the “why” behind your pain, ensuring your recovery plan is personalised, not cookie-cutter. We perform a detailed physical exam to map your nerve health. This may include: Neural Tension Testing: Straight Leg Raise and Slump Tests to gauge nerve irritability. Motor & Sensory Check: Assessing big toe extension and gait (heel/toe walk) for signs of weakness. MRI Review: We review your scans, but we treat the person, not the image. We identify your Directional Preference. By testing how your pain responds to specific spinal movements (flexion vs. extension), we find the “mechanical key” that centralises your pain and provides immediate symptomatic relief. This is where we bridge the gap between “hurt” and “harm.” You won’t just get a generic exercise sheet. You will receive real-time coaching on: Neural Mobilisation: “Flossing” the nerve to reduce hypersensitivity and improve muscle activation. Foundational Patterns: Learning to hip hinge and squat without triggering symptoms. Fear-Avoidance Reduction: We teach you which movements are safe to push through, empowering you to move with confidence again. You leave your first session with a clear, actionable plan. No vague advice to “rest and ice.” You get: Immediate Relief Strategies: What to do when pain flares at your desk. Office Ergonomics: How and when to sit or move during your workday in the CBD. The Loading Protocol: The exact exercises you need to start building capacity today. The most common question we receive at our Singapore clinic is: “How many sessions until I’m pain-free?” While every nervous system is different, we generally see results move through three distinct phases. Phase 1: Symptom Management (Weeks 1–2) Phase 2: Active Loading (Weeks 3–6) Phase 3: Resilience & Discharge (Weeks 7–12+) Centralisation Speed: If your pain responds quickly to directional preference testing, your timeline is usually shorter. Tissue Health: Chronic cases (over 6 months) require more patience than acute flare-ups. The “Active” Variable: Recovery is a partnership. Consistency with your daily loading exercises and providing clear, detailed feedback on your symptoms allows us to fine-tune your program effectively. This communication is the #1 predictor of a fast discharge. At Square One, our goal is to discharge you, not keep you on a lifelong treatment plan. If you are required to see a chiropractor indefinitely just to “keep the pain away,” the treatment is likely failing to build your actual physical resilience. We don’t settle for temporary relief. We aim for permanent independence. If you work in the CBD Raffles Place or live near Chinatown or Outram Park, you need a sciatica chiropractor who understands your specific aggravators. Recent reports from Singapore General Hospital show that younger professionals are increasingly affected by sciatica due to sedentary desk work and poor posture: We’re positioned to be accessible from the city’s central districts so you can fit treatment into your lunch break or before/after work. Convenience matters when you’re trying to stay consistent with treatment without derailing your entire day. While most cases of sciatica respond well to active recovery, you should go to the Accident & Emergency (A&E) department immediately if you experience: These are signs of cauda equina syndrome or other emergencies requiring surgery. We work closely with orthopedic and neurosurgical specialists in Singapore and will refer you immediately if needed. Is chiropractic care safe for sciatica? Yes, when practiced using evidence-based methods. We avoid high-velocity manipulation during acute flare-ups and focus on neural mobilisation and graded exercise instead. Can sciatica go away on its own? Sometimes. About 50% of cases improve within 6 weeks without treatment. But recurrence rates are high if the underlying movement dysfunction and weakness aren’t addressed. If your pain has been persisting for more than 6 weeks, it’s unlikely it will improve on its own without professional help. Should I get an MRI before seeing a chiropractor for sciatica? Not necessarily. MRI is recommended if there are red flags (see above) or you’re actively considering surgery. We can often diagnose and treat effectively without imaging. What’s the difference between sciatica and piriformis syndrome? Piriformis syndrome involves compression of the sciatic nerve by the piriformis muscle in the buttock. True piriformis syndrome is rare. Most “piriformis” diagnoses are actually radiculopathy from the spine. Our assessment distinguishes between them. Will I need surgery for my sciatica? Surgery is rarely the first option. Studies show that conservative care (like our approach) produces similar outcomes to surgery for most cases at 1-year follow-up. Surgery is reserved for severe, progressive neurological deficits or cauda equina syndrome. “Do you provide physiotherapy for sciatica?” While Square One is a chiropractic clinic, our approach is heavily rooted in physiotherapy-based active recovery. We believe that for sciatica, a chiropractor’s expertise in spinal health is most effective when paired with the exercise rehabilitation found in modern physiotherapy. If you’re searching for a sciatica chiropractor in Singapore who treats the nerve, not just joint misalignments or so called “chiropractic subluxation”, you’ve found the right place. At Square One Active Recovery, we’re not interested in endless “maintenance.” We’re here to: Conveniently located in Chinatown near Raffles Place and Outram Park, we make it easy to fit evidence-based sciatica care into your schedule. Based in Singapore, Square One Active Recovery offers treatments with a very big difference. With our evidence-based exercise approach, you can achieve your recovery goals in just 12 weeks. Not getting results from your chiropractor, TCM doctor or physiotherapist? Talk to us and find out how we can take your recovery to the next level. Our goal? To make our own services redundant to you. *We do not offer temporary pain relief such as chiropractic adjustments, dry needling, or any form of soft tissue therapy.
💡 At a Glance: Sciatica Recovery in Singapore
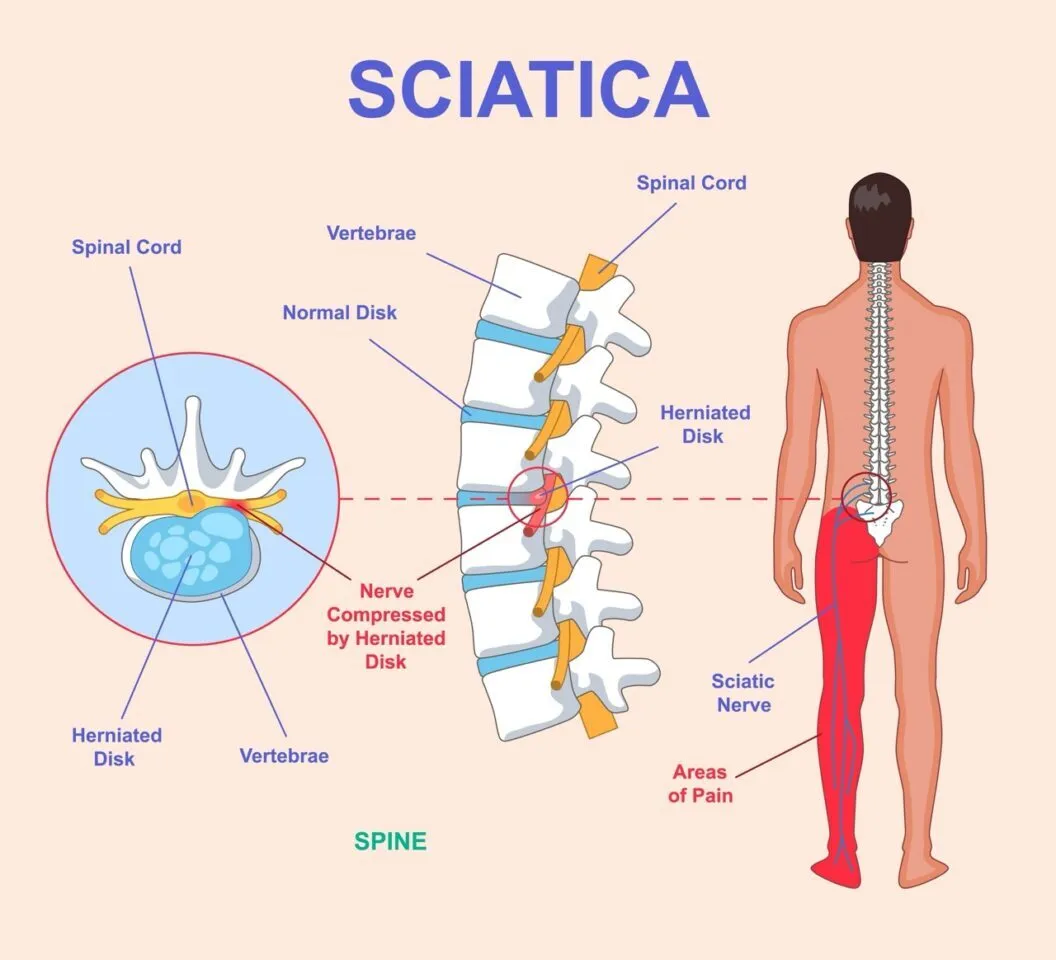
What is Sciatica? (The Neurological Perspective)
Common Symptoms of Lumbar Radiculopathy in Singapore Patients
Sciatica vs. Back Pain: How to Tell the Difference
Feature
Sciatica (Lumbar Radiculopathy)
Mechanical Back Pain
Pain Location
Radiates from lower back/glute down the leg to the foot.
Localised strictly to the lower back area.
Sensation
Sharp, shooting, electric, or burning sensations.
Dull, achy, or stiff sensation.
Neurological Signs
Numbness, tingling, or muscle weakness in the leg/foot.
Usually absent; no nerve-related symptoms.
Triggers
Worsens with sitting, coughing, sneezing, or specific leg movements.
Worsens with certain postures, lifting, or prolonged standing.
Nerve Involvement
High (Involves the sciatic nerve, the body’s largest nerve).
Low (Typically involves muscles, ligaments, or joints).
Treatment Focus
Neural desensitisation and active loading.
Progressive overload and core stability.
Why Traditional Chiropractic “Adjustments” Often Fail for Sciatica
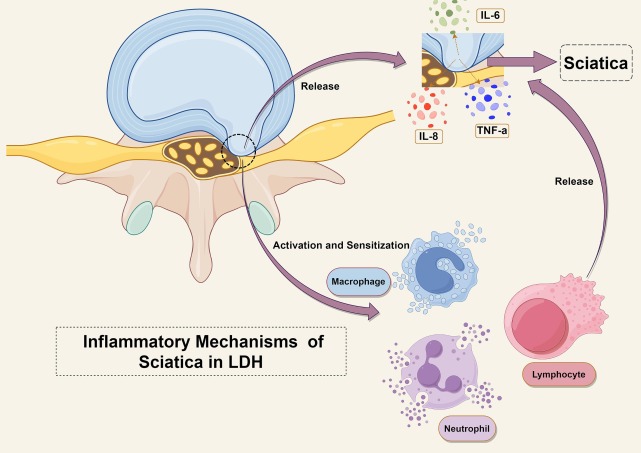
Disc Herniation and Sciatica: The Mechanical-Chemical Double Hit

The Square One Method: Neural Desensitisation & Active Loading for Sciatica
1. Neural Desensitisation (Calming the Nervous System)
2. Progressive Load Tolerance (Building Capacity and Resilience)
Why Permanent Results Require More Than Adjustments
Your Recovery Journey: From Pain Relief to High Performance
1. Clinical Consultation: Understanding Your Story
2. Comprehensive Neurological Assessment
3. Movement Provocation & Relief Testing
4. Supervised Exercise & Movement Retraining
5. Your Roadmap to “Antifragility”
How Long Does Sciatica Treatment Take?
Your Recovery Timeline
Focuses on “lowering the volume” of the nerve. Most patients see significant pain reduction and improved movement tolerance within 2–3 sessions.
Once the pain centralises (moves from the leg back to the spine), we begin building capacity. This involves weekly sessions to ensure you are loading the spine safely.
This is where we transition to bi-weekly or monthly check-ins. The goal is a return to full function and usual activity. With strength and conditioning, you can go to the gym or work long office hours without worrying about a relapse.Factors That Influence Your Speed of Recovery
Our “Exit Strategy” Philosophy
Why Location Matters: Sciatica Treatment Near Chinatown, CBD, and Raffles Place
Red Flags: When Sciatica Requires Immediate Medical Attention
❓ Frequently Asked Questions About Sciatica Chiropractic Care
Start Your Sciatica Treatment Today
BOOK A CHIROPRACTOR IN SINGAPORE
Categories