Low back pain is one of those funny conditions where it is never too serious on its own. It’s not like cancer or heart diseases that can lead to death if untreated. But yet lower back is extremely difficult to live with. In fact, lower back pain the leading cause of disability worldwide.
There are many treatments for back pain available in Singapore. Today, we will focus mostly on back pain treatment from a chiropractic approach.
What is low back pain?
Strictly speaking, low back pain will refer to pain coming from the spine between the L1 and L5 vertebrae as well as the surrounding tissues. In the context of acute injuries, pain can originate from the joints and muscles in the lumbar region.
In chronic cases however, it is impossible to identify a single source that is causing the pain. Research has repeatedly demonstrated that chronic pain is multifaceted in nature and there is no single cause for it. This is why a lot of treatments for back pain fail, in the sense that your pain may improve but will come back over and over again.
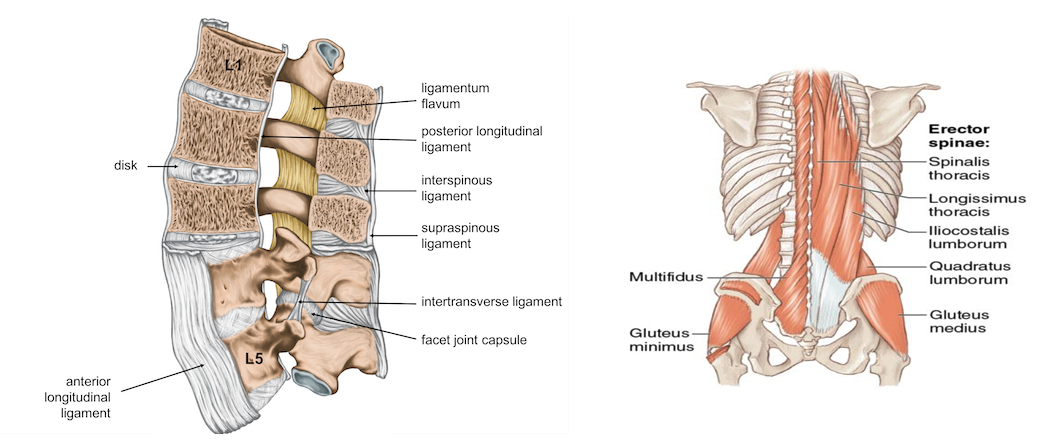
Joint sprains and muscle strains are most common causes of acute low back pain. The facet joints are the ones most commonly affected (i.e., facet joint capsule). The facet joints connect the vertebra to the vertebrae above and below it. They can be found on both sides of the spine.
Muscle strains are also fairly common. After a hard squat or deadlift session, you may feel some aches in your low back. This ache is usually coming from the lumbar paraspinal muscles (e.g., erector spinae) or the quadratus lumborum.
Other types and sources of low back pain is often more complex in nature and will need professional diagnosis.
Why Choose a Back Pain Chiropractor in Singapore?
You will be surprised to learn that a medical doctor is probably not the best person to see for back pain. Back pain is considered a musculoskeletal condition and is better treated by chiropractors or physiotherapists.
Although chiropractors are not recognised in Singapore, they are experts in musculoskeletal conditions. Did you know Jesse, our chiropractor at Square One Active Recovery, spent five years in chiropractic school to qualify as a chiropractor? All five years of his training was spent solely on musculoskeletal conditions. In comparison, physiotherapy school is only four years in Singapore. Their training is also more general as they have to cover other domains such as neurology and cardiorespiratory diseases.
According to Harvard Medical School, back pain sufferers experience less pain and less disability after six weeks of chiropractic treatments.
When should I see a GP for back pain?
Family doctors or general practitioners are probably the best doctors to see if you are looking to get some prescription medication. Most doctors in Singapore will prescribe you with anarex, which is a type of muscle relaxant that also helps with pain.
If you require a referral letter from your insurance company, a medical doctor can also issue you with one.
Virtually all clinical guidelines do not recommend medication as firstline treatment. As such, it may not be necessary to see a doctor for your back pain.
Can a chiropractor fix back pain?
If you check out our Google reviews, you will see a lot of our clients had success with us for their back pain treatment. This is because chiropractors do focus more on conditions of the spine.
There are concerns that because chiropractic is unregulated in Singapore, chiropractic treatments are unsafe or does not work. This is not true.
A lot of concerns regarding safety of chiropractic is blown out of proportion by the media. It is true that there are reports of deaths following chiropractic adjustments, and we have written about them before. However, this doesn’t mean the chiropractors caused the stroke.
For example, in the case of Joanna Kowalczyk, the coroner report suggested that she likely suffered the first vertebral artery dissection (which later led to a stroke) during her personal training session.

There are of course chiropractic techniques that are more dangerous than others. Evidence-based chiropractors will never perform y-strap vs ring dinger adjustments. From an anatomical point of view, such manipulation techniques just doesn’t make sense and is mostly made popular by good marketing and social media.
What is evidence-based chiropractic?
The truth is that there are evidence-based chiropractors in Singapore. You just need to know where to look. Our treatments at Square One Active Recovery are aligned to all clinical guidelines. Biases aside, we would be considered an evidence-based chiropractic clinic.

Our primary goal is to help get them stronger, fitter, and more functional with their bodies. Following which, we work with our clients to get the necessarily lifestyle changes in place so they can have long-term results.
What will an orthopedic surgeon do for back pain?
Seeing a orthopaedic surgeon for any form of muscle or joint pain without first trying out conservative care is not ideal. This is not only our opinion but all international guidelines on chronic pain reflects this.
This is because the success rate of orthopaedic surgery is not as high as where we would want them to be, especially given the risks that are inherent with all surgeries. This is not something that is well discussed by the mainstream media or medical professionals.
Poor outcomes are so well reported that there is a special term for this situation: failed back surgery syndrome (FBSS). FBBS refers to the condition where pain persists after surgery or resurfaces later after surgery. Failed back surgery syndrome is estimated to affect 10-40% of all back surgeries.
There is currently no cure for FBSS though neurosurgeons can perform revision spine surgeries which may help.
What are the 3 common causes of back pain?
One of the leading causes of back pain is muscle strain or sprain. This often occurs due to overtraining, improper lifting techniques, sudden movements, or overexertion, or deconditioning due to sedentary lifestyle. Strained muscles can cause focal pain and stiffness, making it difficult to perform daily tasks.
How do I know if I’ve herniated my disc?

Herniated discs, also known as slipped or ruptured discs, occur when the soft cushion-like discs between the vertebrae bulge or rupture. Disc herniations can sometimes cause sharp or shooting pain, numbness, and tingling sensations in the back and legs. There may be a weakness in the lower extremity muscles. For more information, check out our Slipped Disc Guide.
You should be mindful that in true disc herniation cases, the leg symptoms is often worse than their back pain. In fact, it is entirely possible to have sciatica nerve pain without any symptoms in your lower back.
What causes spinal stenosis?

Spinal stenosis refers to a condition characterised by the narrowing of the spinal canal. Most spinal stenosis are cause by age-related changes in the spine that result in changes in the structure of the spine.
This can result in pressure on the spinal cord and nerves. This narrowing often occurs due to the age-associated changes of spinal structures (e.g., bones, discs, or ligaments). Spinal stenosis typically manifests as pain in the lower back and legs. The pain often worsens with walking or prolonged standing and feels better with forward bending or slouching. This is sometimes called the shopping cart sign.
How serious is osteoarthritis of the spine?
Often inaccurately referred to as the wear and tear of the spine, osteoarthritis is now understood to be a normal age-related process. Like how your white grey doesn’t give you headache and your wrinkles don’t give you face pain, osteoarthritis is poorly correlated with back pain.

A study of over 3,000 asymptomatic participants (i.e., no low back issues whatsoever) found that osteoarthritic changes are common even in painless people. Over a third of young adults (in their 30s) with no back problem would start to show signs of degeneration. This figure increases to 96% for those in their 80s.
You can see from the table above that as you grow older, you are more like to get degeneration. This much is true. However, these people have no pain!
One of the best thing you can do to prevent degeneration of the spine is exercise! Previous studies have reported that people with a sedentary lifestyle are more likely to have osteoarthritis than people who are active.
How do I know if my back pain is from posture?

Many of us have been advised by our parents, teachers, or even healthcare professionals to maintain “good” posture to prevent pain. However, it’s time to debunk these myths and shed light on the scientific evidence that challenges the notion that posture is a direct cause of pain.
Contrary to popular belief, there is limited scientific evidence to support the idea that poor posture directly causes pain. Conversely, there is robust research to show on association between posture and any form of physical health.
Anterior pelvic tilt is also a topic that frequently surfaces. However, it does not automatically cause pain. Both anterior and posterior pelvic tilts can be considered normal postures.
What is the best exercise to relieve lower back pain?
Exercise therapy plays a vital role in managing back pain. In Singapore, numerous clinics and rehabilitation centers offer specialised programs to help patients strengthen their muscles, improve flexibility, and find freedom from pain. However, there is no single best exercise for back pain.
Engaging in regular physical therapy sessions such as pilates that are customised to your condition can enhance your overall back health and promote long-term recovery.
While exercise is often associated with physiotherapy, exercise is very much part of chiropractic since its founding days.
In the picture above, you can see lots of exercise equipment. This is in fact BJ Palmer’s chiropractic clinic. He is the son of DD Palmer — the founding father of chiropractic — and is guy who made chiropractic what it is today.
You can see that he has a stationary bike, rowing machine, and even a punching bag!
It is true that chiropractors in Singapore tend to focus to spinal manipulation. However, exercise is very much also considered chiropractic treatment.
Does chiropractic really help back pain?
For the past 15 years I have been going for the usual chiropractic adjustment for my neck and back pain and I was seeking a long-term sustainable solution when I came upon Square One Active Recovery. I decided to sign up for the program as it ticks all the boxes – no chiropractic adjustments, don’t need to depend on anyone and don’t have to keep coming back. I am very happy with the results of the program as I am now free from chiropractic adjustment, my overall strength and endurance have improved and I am better able to perform many day-to-day tasks.
Traditional chiropractors believe that chiropractic subluxations are the common cause of neck symptoms. Their approach to your pain consequentially revolve around treatments to remove subluxations. However, no reasonable quality research to date has been able to demonstrate the existence of chiropractic subluxation. In addition to that, results with subluxation-based chiropractors tend to be temporary. It is not uncommon to hear about them selling packages with over 40 sessions. You are also usually required to come back for life under a wellness or maintenance plan.

Unfortunately, chiropractic adjustments simply don’t work. Recent research is able to demonstrate that spinal manipulation is no better than placebo! This research is also performed by chiropractors (i.e., not other healthcare providers trashing chiropractic).
This doesn’t mean a chiropractor cannot help you! Evidence-based chiropractors are completely different from the traditional chiropractors. We take into consideration the latest research on what works the best for your neck pain.
Because we are willing to adapt and embrace the latest research, we offer more than just spinal adjustments. As a result, you get better results with us than traditional chiropractors.
What are the lifestyle factors of back pain?
In addition to an evidence-based exercise programme, incorporating lifestyle modifications can play a significant role in effectively managing back pain. By making positive changes to your daily habits and routines, you can enhance your overall well-being and alleviate discomfort. Here are some key lifestyle modifications Square One Active Recovery can help you with:
- Maintaining a healthy weight
- Having a healthy relationship with food and eating
- Getting enough sleep ever night
- Participating in regular exercise
- Cultivating a good social life
- Sensible sitting or standing Behaviour:
Jesse is a certified solution-focused coach. Instead of dwelling on problems and giving prescriptive blanket advice, Jesse guides clients towards identifying their strengths, resources, and the possibilities for positive change. In sessions with Jesse, clients can expect a collaborative and supportive environment. Jesse works with clients to co-create strategies and action plans that align with their unique circumstances and aspirations. By exploring clients’ desired outcomes and helping them envision their preferred future, Jesse empowers individuals to take actionable steps towards achieving their goals.
How can I promote a healthy spine?

Our ethos has always been clear. We want to make our own services redundant to you. Our methodology to pain management is designed around an empowerment model so there is no dependency on us.
We use exercise to help you help yourself work on your own physical body. We don’t just stop there! We also educate you so you are knowledgeable and skilled to own self help own self. As as solution-focused coach, Jesse is also able to partner you to get to the health habits you have been struggling to attain.
Dealing with back pain can be a debilitating experience, but finding effective solutions is possible in Singapore. By working with an evidence-based chiropractor, you can regain control over your back health. Remember, each individual’s experience with back pain is unique, so it’s essential to work closely with professionals to determine the most suitable treatment plan for your specific condition.
Don’t let back pain hold you back—drop us a message to learn more about the first step towards a pain-free life today!
BOOK A CHIROPRACTOR IN SINGAPORE
Based in Singapore, Square One Active Recovery offers treatments with a very big difference. With our evidence-based exercise approach, you can achieve your recovery goals in just 12 weeks. Not getting results from your chiropractor, TCM doctor or physiotherapist? Talk to us and find out how we can take your recovery to the next level.
Our goal? To make our own services redundant to you.
*We do not offer temporary pain relief such as chiropractic adjustments, dry needling, or any form of soft tissue therapy.


